Elucidation of metabolism of the anticancer drug lenvatinib as a possible path to personalized therapy
Have you wondered why it is important to know the metabolism of lenvatinib, or the fate of this drug in the body? It is largely due to the possible use of drug combinations in anticancer therapy, in order to make it more efficient. Cytochromes P450 (CYPs) are key enzymes involved in drug metabolism. The risk of drug interactions rises from possible induction of these enzymes or from the simple fact that if two or more substances that are substrates of these enzymes are administered simultaneously, they may compete for the same enzymes. These interactions can subsequently lead to various side effects or to a reduction in the activity of the drugs used.
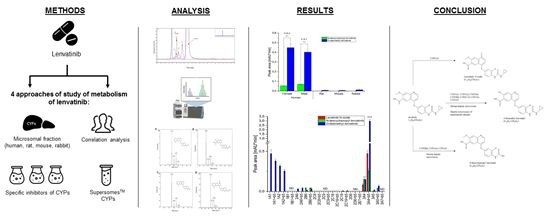
In our in vitro study, we used several approaches to identify lenvatinib metabolites and to identify specific enzyme isoforms responsible for this metabolism: incubation of lenvatinib with animal or human liver microsomes, addition of inhibitors of individual cytochrome P450 isoforms to the incubation mixture or incubation with recombinant human enzymes. Previous studies by Japanese pharmaceutic company Eisai suggest that lenvatinib is extensively metabolised by CYP3A4. However, our results provided a new perspective on metabolism and indicated a significant role for CYP1A1. This isoform was even identified as more active compared to CYP3A4 in the absence of cytochrome b5. This knowledge may serve as a basis for future studies focusing on drug interactions associated with CYP1A1, not just CYP3A4 as described in previous publications.
Document Actions